The Risks for Women of Color
By IRENE SPEZZAMONTE, VANESSA SWALES and KAITLIN SULLIVAN
Childbirth in America is more dangerous for women from minority groups — especially in New York City, where black women are 12 times than white women to die of pregnancy-related causes, city data show.
New York City “is an incredible outlier,” worse than elsewhere in the country for African-Americans, according to William Callaghan, chief of the maternal and infant health branch at the U.S. Centers for Disease Control. Nationally, black women are three to four times more likely to die of pregnancy-related causes than white women. Callaghan has studied maternal health for four decades and has seen that gap throughout his career, he said.
“It’s consistent, it’s pernicious,” he said. “We haven’t made a dent in the disparity.”
The disparity transcends class and education: Black New Yorkers with a college education are three times more likely to experience serious complications in pregnancy than white women in the city who have not graduated from high school, city Department of Health statistics show.
Overall, death in pregnancy is rare and serious complications are uncommon: About 30 New Yorkers every year die from pregnancy-related causes, and more than 3,000 women face life-threatening complications out of about 120,000 births in New York City in 2016, city Health Department data show. But those who live in poorer neighborhoods, and women of color, face greater risks.
The reasons for the racial imbalance in birth outcomes are complex, experts say, and include unequal access to health insurance and prenatal care; pre-existing health factors such as hypertension and diabetes that disproportionately affect pregnant women of color; and, some argue, the corrosive effects of structural racism — which former city Health Commissioner Dr. Mary Bassett defined as “inequitable distribution of resources across neighborhoods and unequal treatment within health care settings.”
But a key factor is the hospitals where women deliver their babies.
In New York City, maternal outcomes vary widely among hospitals, with the risk of severe complications ranging from 0.8 percent up to 5.7 percent, according to one study. That risk holds even when adjusted for the health of expectant mothers at the time they entered the hospital doors.
Dr. Elizabeth Howell, who runs the Blavatnik Family Women’s Health Research Institute at Mount Sinai Hospital, found in the study that almost two-thirds of white women gave birth in the city’s low-risk hospitals, compared to 23 percent of black women. Only 18 percent of white women gave birth in high-risk hospitals, while 37 percent of black women delivered in those hospitals.
Speaking at a maternal health symposium in Newark, New Jersey, last November, Howell said differences in hospital quality may account for nearly half of the disparity in maternal experiences between black and white women. She did not name which New York hospitals are low risk versus high risk and declined an interview request.
Teaching hospitals, which prepare the next generation of doctors, tend to perform better, she said at the symposium. But that is not the sole explanation of the gap in maternal experience.
“White women are getting better care in hospitals where they go,” said Dr. Leslie Farrington, a retired ob-gyn who is the founder of ASK for Your Life, a health-care advocacy group. “White patients don’t go to Jacobi (Medical Center, in the Bronx) to deliver. That’s part of the segregation.”
Farrington said the care provided by staffs at hospitals of lesser quality suffers because of lack of resources and sometimes because of staff attitudes toward the patients. “I believe a lot of it has to do with not paying attention to the patients, time pressures, work pressures,” she said. “Their decisions and their behaviors are affected by their biases when they are under pressure.”
Severe maternal morbidity (SMM) in NYC in 2013-2014, by background factors
Based on matching birth certificate data from the New York City Department of Health and Mental Hygiene Bureau of Vital Statistics to hospital discharge records from the New York Statewide Planning and Research Cooperative System (SPARCS) for all NYC hospital deliveries in 2008-2014. Source: New York City Department of Health and Mental Hygiene
In Central Brooklyn, high rates of complications
New York’s poorest and largely black neighborhoods, like Brownsville and East Flatbush in Brooklyn, are among those with the highest rates of pregnancy-related complications.
In Brownsville, for instance, life-threatening complications occur in 497 of every 10,000 deliveries. In nearby East Flatbush the rate is almost as high. The levels are nearly four times higher than in affluent and predominantly white neighborhoods like Battery Park, Greenwich Village and Park Slope, city Department of Health numbers show.
Pre-existing health factors can play a role. Black New Yorkers experience higher rates of obesity and diabetes — conditions that can be linked to adverse outcomes during childbirth.
While outcomes are improving for women who suffer from embolisms and hemorrhaging during pregnancy, complications because of cardiovascular problems are rising, especially among African-American women.
Dr. Kecia Gaither, director of perinatal services at Lincoln Hospital in the Bronx, said physicians who work with African-American patients need to be aware of health problems. Gaither works with expectant mothers to improve their nutrition, and she screens those with warning signs for hypertension.
“Having a working knowledge of the population that you serve,” she said, “is really important in taking care of this high-risk population.”
The city is trying to attack the problem by working with community organizations to provide education. Health Action Centers provide perinatal care in Brownsville, East Harlem and Tremont in the Bronx. In Brownsville, parents-to-be can learn more about medical insurance, take childbirth classes and take yoga classes.
The city is funding groups like the Birth Justice Defenders, which gives mothers a place to discuss problems they have faced in deliveries.
“Being listened to and trusted and having your pain and symptoms taken seriously, and being included in the decision-making process for what happens to your body and your baby – all of that plays into having good birth outcomes,” said Silvia Beltran, the program’s coordinator.
But Aletha Maybank, associate commissioner at the Center for Health Equity in the Department of Health, said it’s challenging to make those programs work in parts of the city as different as Brownsville and Staten Island. And they need to be embedded in larger systems of health, housing and transit, she said. “In terms of long-term closing of the gaps, that will take a pretty long time,” she said.
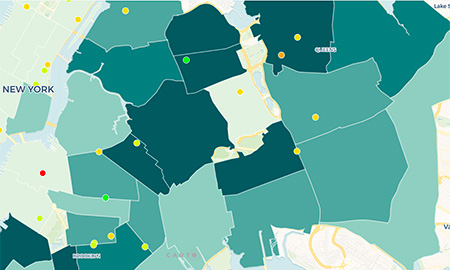
Severe maternal morbidity (SMM) in NYC in 2013-2014, by community district
Source: New York City Department of Health and Mental Hygiene. Based on matching birth certificate data from the New York City Department of Health and Mental Hygiene Bureau of Vital Statistics to hospital discharge records from the New York Statewide Planning and Research Cooperative System (SPARCS) for all NYC hospital deliveries in 2008-2014.
For Latina women, lack of insurance affects care
Hispanic women are three times more likely than white, non-Hispanic women to die from pregnancy-related causes and rank among the communities with the highest rates of serious pregnancy complications in the city, according to a 2016 study published by the New York City Department of Health and Mental Hygiene.
Latina mothers in the city face far grimmer outcomes than in the rest of the United States, where Hispanics tend to have better results than white women, the study found.
A key factor is lack of health coverage. Twenty-two percent of Latino adults in New York City are uninsured, according to a report released this year by the New York City Department of Health and Mental Hygiene. Puerto Ricans, Mexicans and Dominicans are particularly hard-hit, according to a study conducted in 2017 by Mount Sinai Hospital.
Although the city’s public hospitals provide services to uninsured women, including the undocumented, lack of insurance discourages pregnant women from seeking care. “When women don’t have access to health care before they get pregnant they likely go into pregnancy with conditions that haven’t been treated, like diabetes,” said Nan Strauss, director of policy and advocacy at Every Mother Counts, an international non-profit organization based in New York City.
Ada Nieves, a maternity nurse who worked at Mount Sinai East for 12 years, said she has seen women treated differently because of their insurance status.
She remembers a Latina woman in her 30s who delivered her baby with a cesarean section. The incision got infected and the mother started bleeding internally.
The mother complained about abdominal pain, but her doctor discharged her and did not follow up post-surgery. The nurse believes the lack of insurance was a key reason. Nieves intervened. The doctor sent the mother to the operating room for a second time to repair the bleeding. “We are not afraid to speak on behalf of the patients — especially undocumented mothers,” Nieves said.
A recent study led by Nancy Krieger, a Harvard University professor of social epidemiology, found heightened stress levels among New York City’s Latina mothers giving birth following President Donald Trump’s election.
As a result, New York City, premature births were more likely among Hispanic mothers, especially those from Mexico and Central America, according to her analysis. Among New Yorkers born in the United States, there was no change; the difference was among immigrants.
“People have physiological responses to feeling threatened,” said Krieger.
Haitian-American women have the worst outcomes
Brooklyn alone has more than 80,000 Haitian-Americans, the third highest concentration in the United States. Women who were born in Haiti and gave birth in New York City endure life-threatening complications during these births at over twice the national average. Severe maternal morbidity affects 494 of every 10,000 deliveries among these women. The national average is fewer than 230.
According to Dr. Tovar “Freddy” Winfred, who specializes in high-risk pregnancies in both Haiti and the U.S., the medical problems killing women in Haiti –– which has the highest rate of maternal mortality in the Western Hemisphere––are the same ones that contribute to high rates of maternal mortality among Haitian women living in New York. A key condition is high blood pressure during pregnancy.
“Those pathologies don’t change because the person has changed geographical location,” said Winfred. If a doctor fails to recognize that a Haitian-born woman could be more likely to suffer from high blood pressure, it can create problems, Winfred said. The problem can be treated in the delivery room if hospital staff quickly recognize symptoms and lower a woman’s blood pressure to prevent a stroke.
“You can’t have healthy babies if you don’t have healthy pregnant women,” says Carine Jocelyn, CEO of Diaspora Community Services in East Flatbush, Brooklyn, and a Haitian-American woman herself.
City census data does not differentiate between African-Americans and Caribbean-Americans at the neighborhood level; but the Flatbush neighborhoods are predominantly Caribbean. Foreign-born women from St. Vincent and Barbados have the second and third highest severe maternal morbidity rates in the city.
East Flatbush, where nearly 90 percent of the population is black, and where 53 percent of the population was born outside the U.S., has the highest rate in the city of mothers who receive late or no prenatal care (just under 16 percent, over twice the city average), according to the New York City Department of Health. It also has the second highest percentage of preterm births in the city, at nearly 13 percent of all live births.
By comparison, preterm births are lowest among women living in Midtown Manhattan––5.7 percent––where roughly 97 percent of women receive prenatal care. Almost 70 percent of Midtown residents are white and just 4 percent are black, according to the health department.
Elisabeth Joseph, whose parents are Haitian, became a doula in 2009. She said long wait times at the city’s public hospitals discourage women from seeking prenatal care, especially because for many immigrants, skipping work for a doctor’s appointment is not an option.
“It’s common for women to have to wait for hours to see a doctor for just a few minutes,” she said. “When it happens again and again, they will stop going.”
A Death at Jacobi
Inspection reports reveal tragedies in city birthing wards. >>>
The Risks for Women of Color
Black women are 12 times more likely to die in childbirth than white women in New York City.>>>
How Your Hospital Rates
Check the rates of C-sections and episiotomies at your NYC hospital.>>>
A student-powered service at the Craig Newmark Graduate School of Journalism
Reporters: Vanessa Swales, Irene Spezzamonte, Kaitlin Sullivan, Shaydanay Urbani
Faculty Advisers: Andrew Lehren, Benjamin Lesser, Christine McKenna, Ellen Tumposky
About the Team